Earn Rewards, Get Cash Back
Let our navces Care Guidance Team of Patient Advocates, Nurses, and Physicians help guide you today.
Call Now (833) 4-navces or (833) 462-8237
Instructions for receiving your navces Cash Back Rewards
Your personal medical information is confidential and will not be shared with your employer.
When you see a Green or Yellow High-Value Medical Provider at a Fair Price, you will earn navces Incentive Rewards.

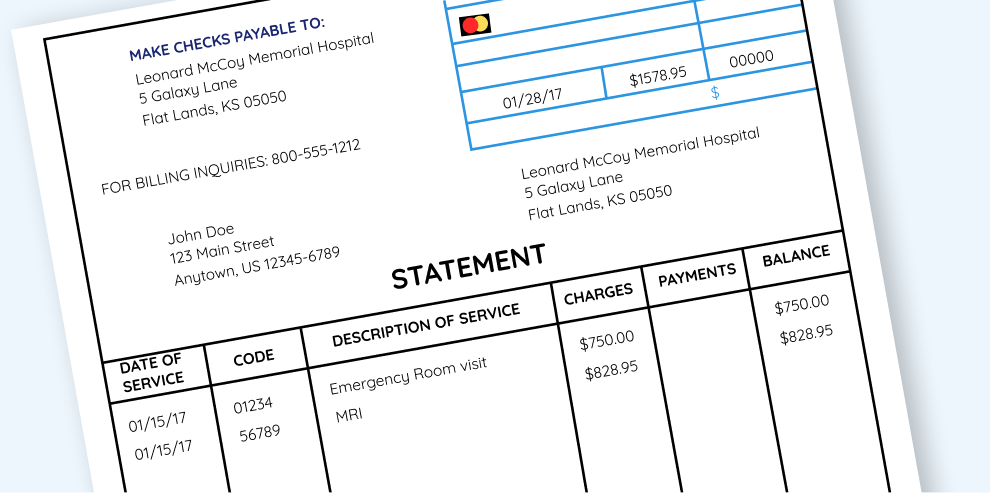
Each time you use your Health Insurance Plan to see a Medical Provider, you are sent an Explanation of Benefits (EOB) by your Insurance Company and will receive an Itemized Medical Bill from your Medical Provider.
Within 90 days of seeing a Green or Yellow High-Value Medical Provider or Facility at a Fair Price, you must provide proof of service with the Green or Yellow provider to navces by submitting your Insurance Provider’s Explanation of Benefits and/or your Itemized Medical Bill.
There are several ways to provide these documents to navces.
- 1 Email a copy to [email protected]
-
2 If you are working with a navces Patient Advocate on
the navces Care Guidance Team, you may provide the
documents directly to your Patient Advocate. -
3 Log onto your account at navces.com and upload
your documents to your Member Account. - 4 Send the documents via secure fax at (786) 471-1078
-
1 Email a copy to
[email protected] -
2 If you are working with a navces
Patient Advocate on the navces
Care Guidance Team, you may
provide the documents directly to
your Patient Advocate. -
3 Log onto your account at navces.com and upload
your documents to your Member Account. -
3 Send the documents via
secure fax at (786) 471-1078
Frequently asked questions
and our best possible answers
Claims data is reviewed on a monthly basis for eligible services, and rewards are issued to qualifying members and dependents.
Rewards should typically arrive at your home within 60 days of receipt by navces of your Insurance Explanation of Benefits and Medical Provider bill.
navces Incentive Rewards are mailed to your home address and will be addressed to the employee, regardless of which family member received care.
Call (833)-4-navces or email [email protected] for more information.
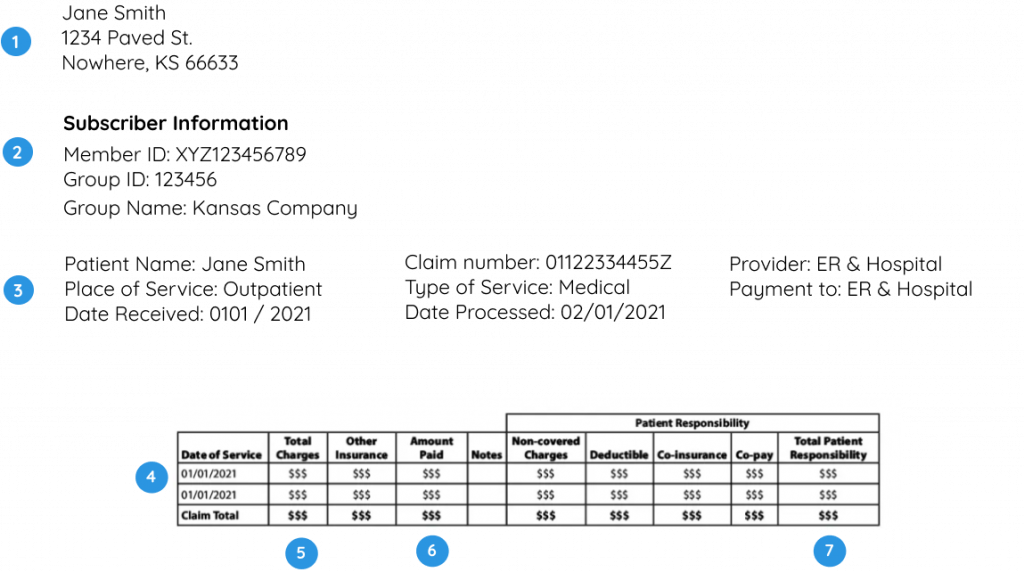
Making Sense of Your EOB
When your insurance company processes your claim, they will send you an explanation of benefits (EOB) detailing what procedures they covered and paid. The most important thing to know about the EOB is that this is NOT a bill. Key- Your name or the insured person’s name and address.
- Your insurance information, such as member ID, group ID, and group name.
- Details about who the patient was, when services were received, what type of services they were, claim information, and provider information.
- Details about the services you received, including but not limited to the date services were provided, the amount your insurance company paid the healthcare provider for those services, any discounts or reductions granted by the insurance company, your deductible and co-payments amounts, and any amounts not covered by insurance.
- The total amount of benefits in the claim.
- The total amount your insurance company is responsible for paying.
- The total of how much you MAY owe, including your co-payments, deductibles, co-insurance, and any amounts not covered by insurance.

